Diagnosis Definition
Branchial Cleft Cyst (BCC)
- The tissues of the neck are embryologically derived from branchial arches and pouches; incomplete arch fusion can result in cysts, fistulas, and sinuses
- Branchial apparatus anomalies (BAAs) are categorized into first branchial cleft cyst, second branchial cleft cyst, third branchial cleft cyst, and fourth branchial cleft cyst types based on location
- 95% of BAAs arise from the second cleft and ¾ of these are cysts, which typically present between 10 and 40 years of age
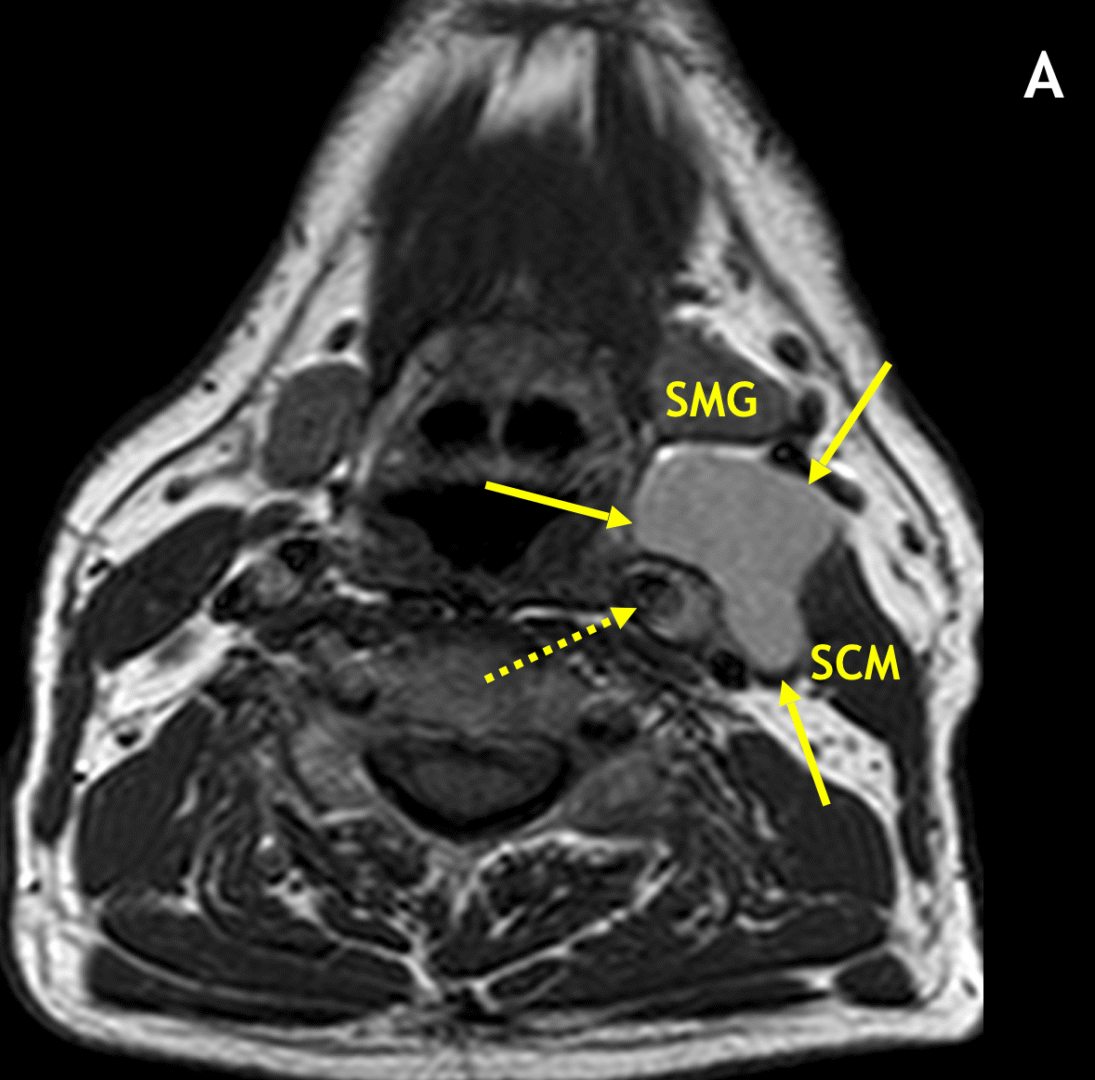
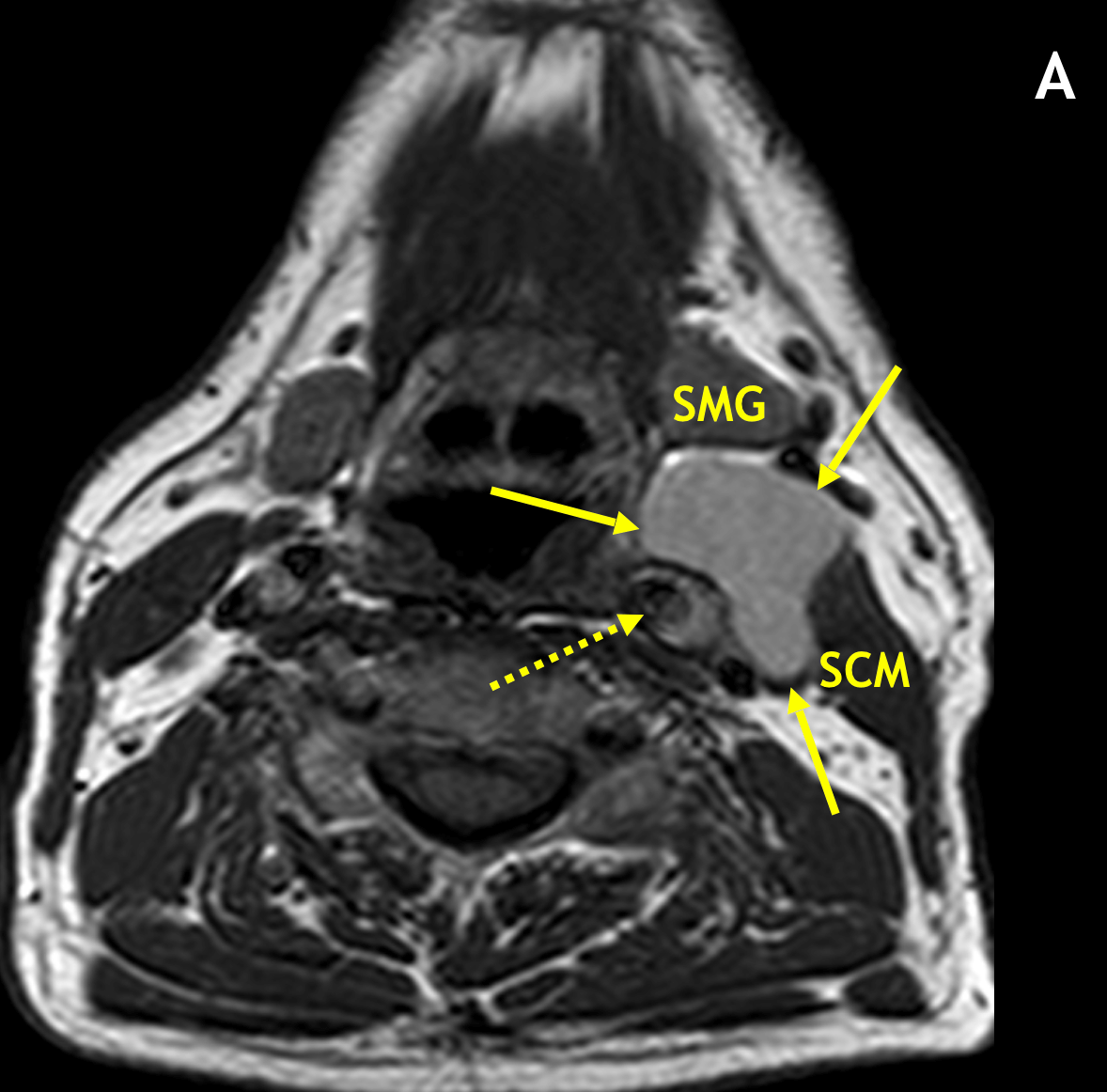
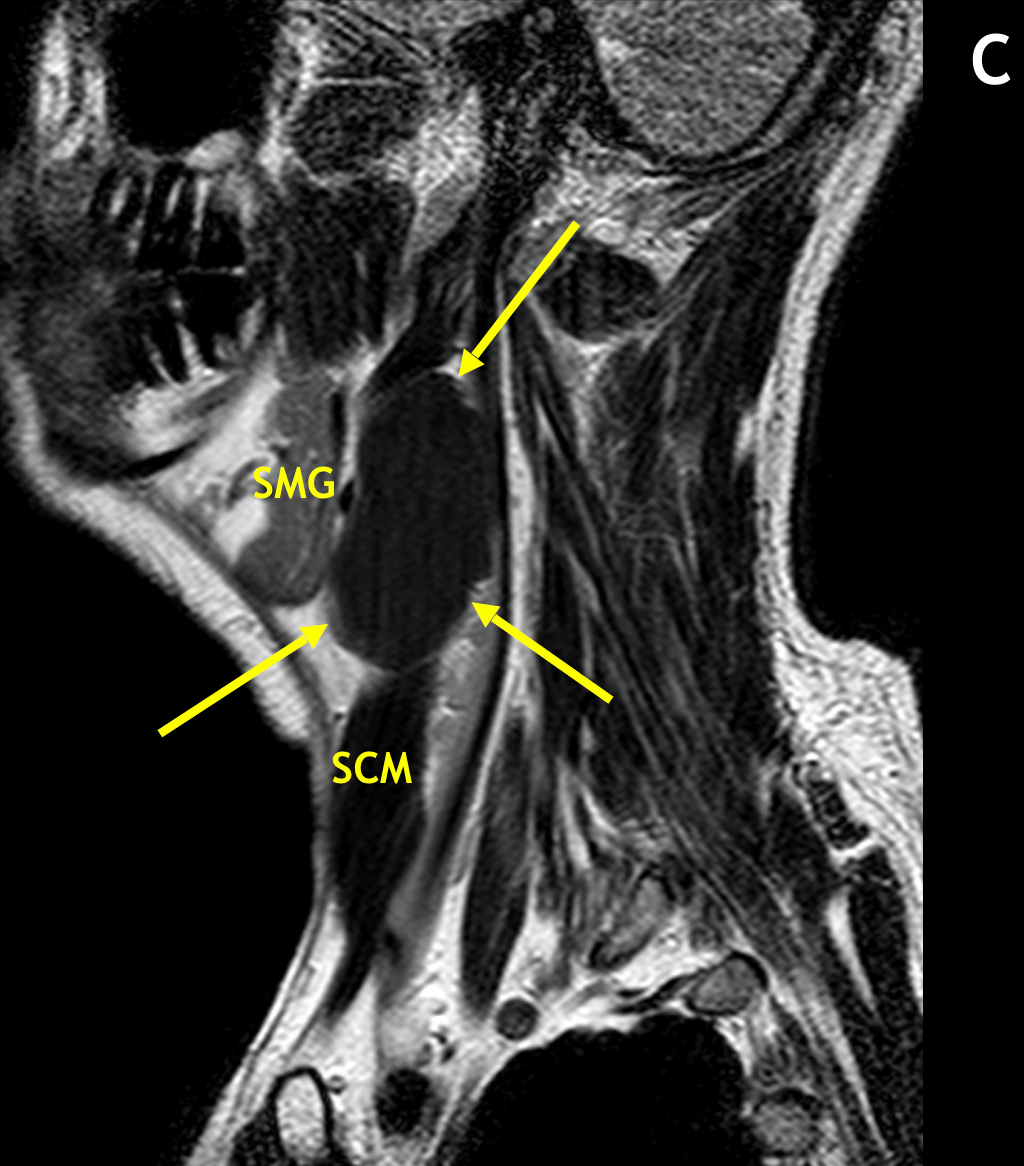
- Second BCCs typically present as a painless, fluctuant mass (neck mass) adjacent to the anteromedial sternocleidomastoid muscle at the mandibular angle, lateral to the carotid space, and posterior to the submandibular gland
- Branchial Cleft Cysts can enlarge slowly over time and become painful if secondarily infected
Imaging Findings
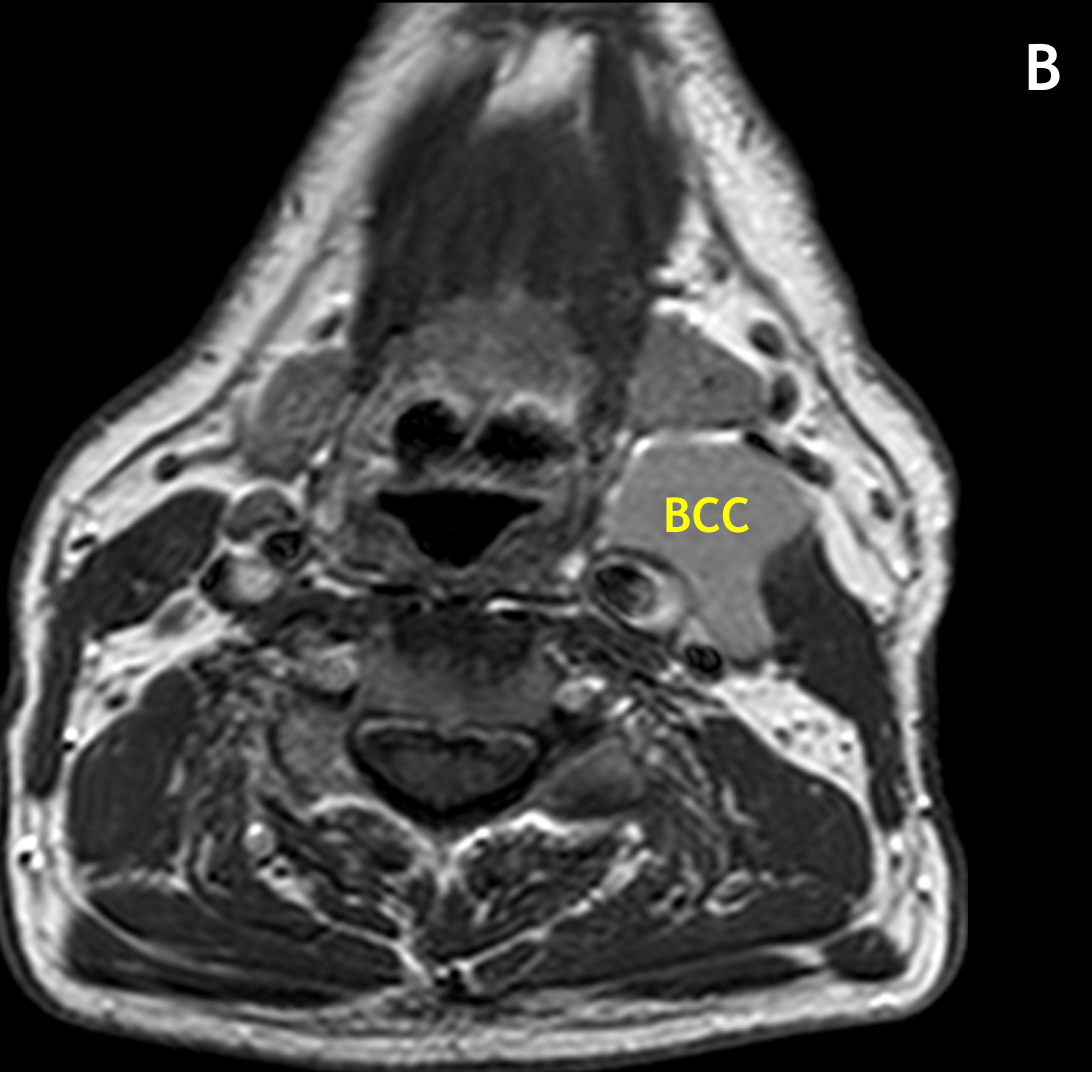
- On MRI, BCCs are seen as circumscribed, round/oval/lobular masses with thin or imperceptible walls
- The signal intensity varies depending on prior infection or hemorrhage, which can result in cysts having high signal on T1 relative to muscle and low signal on T2 due to proteinaceous debris; uninfected BCCs should not enhance
- In the classic location, second BCCs can displace the sternocleidomastoid muscle laterally, the carotid artery medially, and the submandibular gland anteriorly
Pearls
- Surgical excision is the recommended therapy for a branchial cleft anomaly because of the frequency of secondary infection
- In a young patient, a history of recurrent inflammation in the region of the mandibular angle is highly suggestive of a second BCC
- A curved rim of tissue (so-called “beak” sign) pointing medially between the internal and external carotid arteries is considered a pathognomonic imaging feature of one form of a second BCC
References
- Koeller KK, Alamo L, Adair CF, et al. Congenital cystic masses of the neck: radiologic-pathologic correlation. RadioGraphics 1999; 19:121-146
- Mukherji SK, Fatterpekar G, Castillo M, et al. Imaging of congenital anomalies of the branchial apparatus. Neuroimaging Clin N Am 2000; 10:75-93
Case-based learning.
Perfected.
Learn from world renowned radiologists anytime, anywhere and practice on real, high-yield cases with Medality membership.
- 100+ Mastery Series video courses
- 4,000+ High-yield cases with fully scrollable DICOMs
- 500+ Expert case reviews
- Unlimited CME & CPD hours