Diagnosis Definition
- Paragangliomas (also called “glomus tumors”) are rare neuroendocrine neoplasms arising from paraganglionic cells of neural crest origin; most occur in the abdomen and only 3% occur in the head and neck; 2-13% are malignant, 1-3% are hormonally active, and age of onset is most commonly the 4th and 5th decades
- The most common head and neck paraganglioma is the carotid body tumor, which occurs at the carotid bifurcation and typically presents as a painless, slowly growing lateral neck mass
- Other common locations in the head and neck are the jugular foramen (“glomus jugulare”), the middle ear (“glomus tympanicum”), and along the vagus nerve (“glomus vagale”); the term glomus jugulotympanicum is used when the tumor involves both the middle ear cavity and the jugular foramen
Imaging Findings
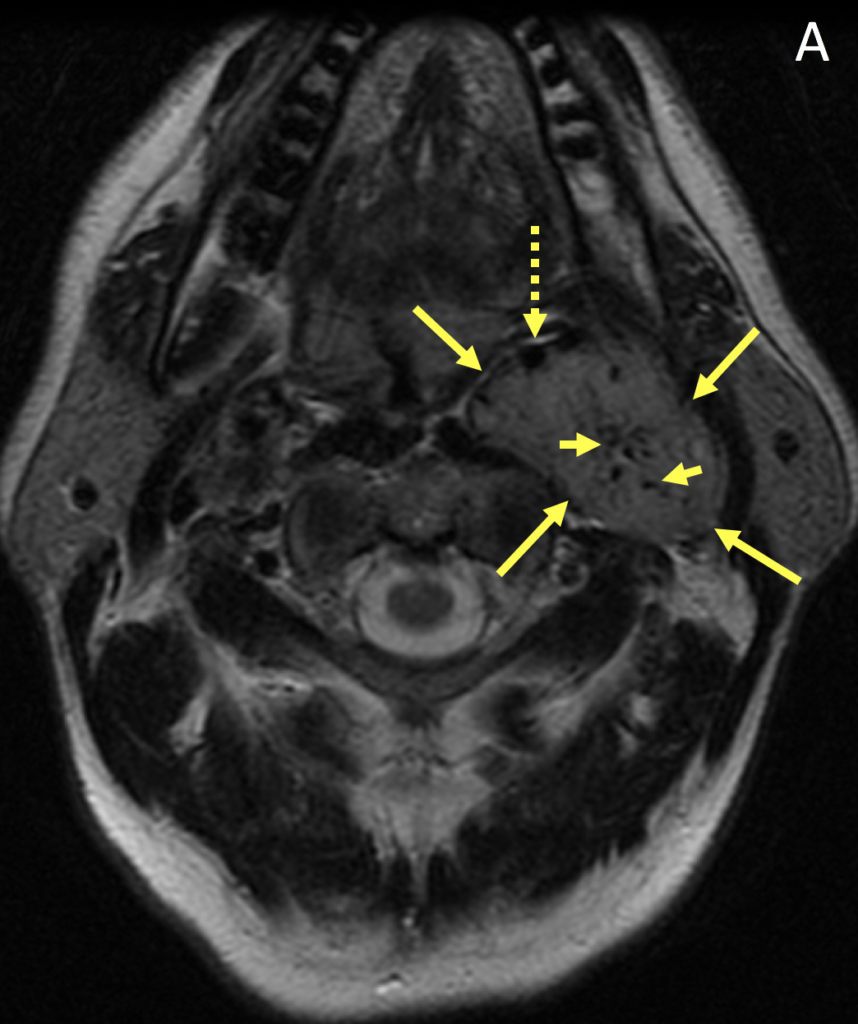
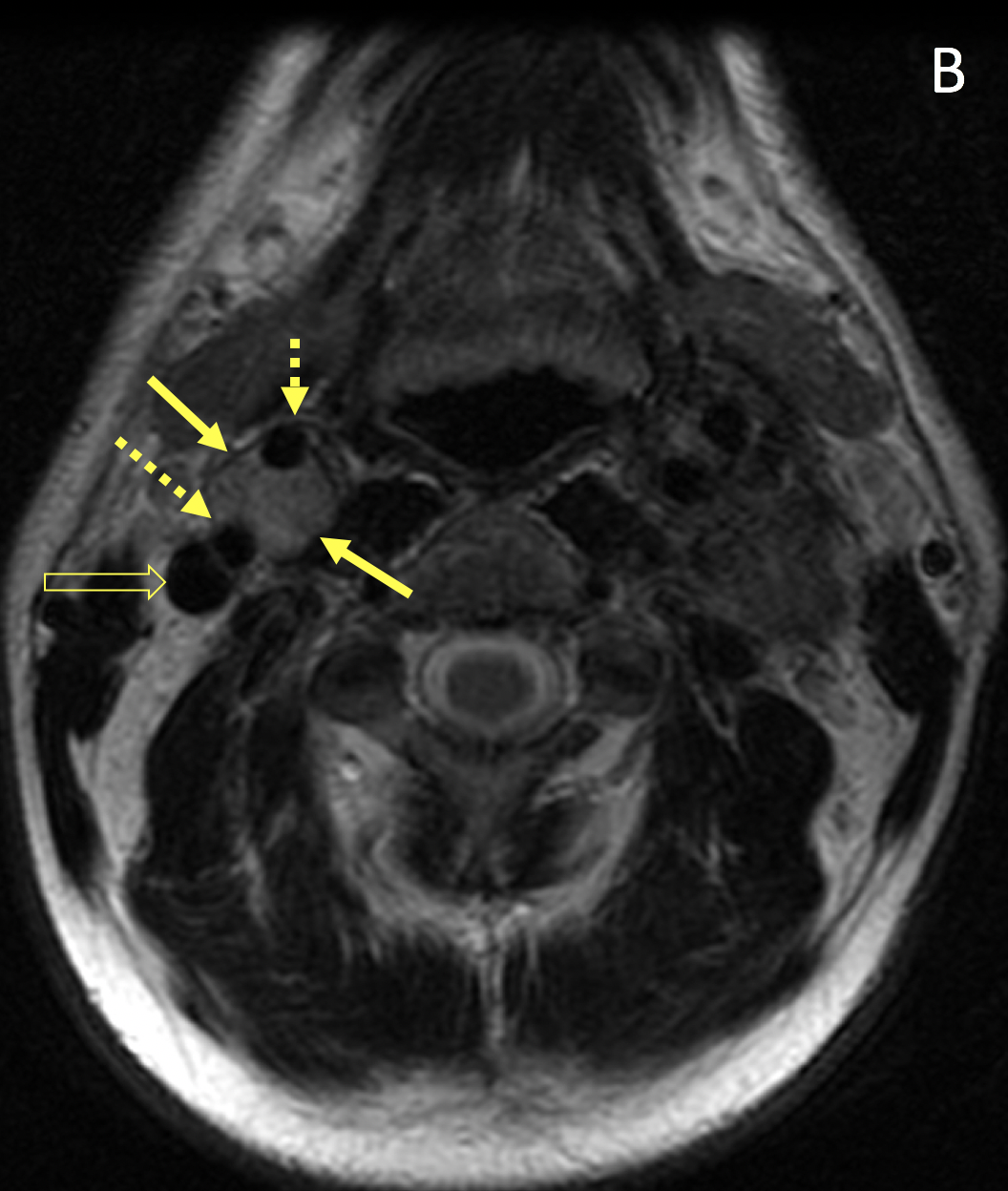
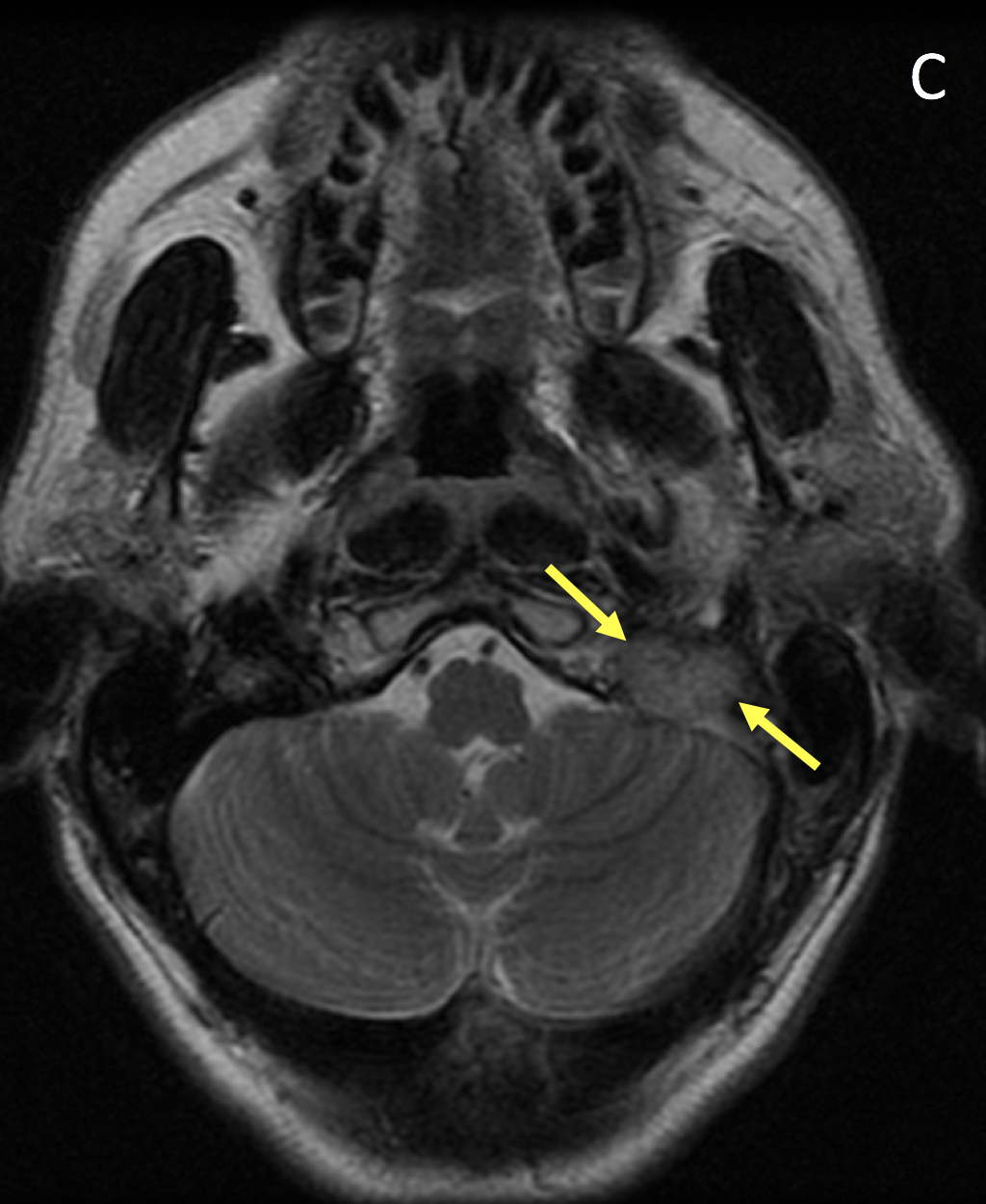
- Paragangliomas are circumscribed, polypoid, hypervascular masses with intense homogeneous enhancement on MRI; early enhancement on dynamic imaging helps distinguish them from meningiomas and schwannomas
- Vascular flow voids can be seen as hypointense foci within the tumor giving it a “salt-and-pepper” appearance
- Splaying of the internal and external carotid arteries is a common feature of a carotid body tumor; as the tumor enlarges, it encases but does not narrow the caliber of the vessels
- Glomus vagale tumors can compress and displace the internal jugular vein posterolaterally and displace the internal carotid artery anteromedially; there is no widening of the carotid bifurcation
Pearls
- In contrast to schwannomas and meningiomas, paragangliomas involving the jugular foramen tend to demonstrate a “moth-eaten” or infiltrative pattern of bony erosion
- About 75% of paragangliomas are sporadic; the remaining 25% are hereditary (and have an increased likelihood of being multiple and developing at an earlier age)
- Familial tumors are commonly associated with multiple endocrine neoplasia (MEN IIA and IIB) and neuroectodermal syndromes (tuberous sclerosis, neurofibromatosis, and von Hippel-Lindau disease)
References
- Rao AB, Koeller KK, Adair CF. From the archives of the AFIP. Paragangliomas of the head and neck: radiologic-pathologic correlation. Armed Forces Institute of Pathology. RadioGraphics 1999; 19(6):1605-1632
- Lee KY, Oh YW, Noh HJ, Lee YJ. Extra-adrenal paragangliomas of the body: imaging features. American Journal of Roentgenology 2006; 187:492-504
Case-based learning.
Perfected.
Learn from world renowned radiologists anytime, anywhere and practice on real, high-yield cases with Medality membership.
- 100+ Mastery Series video courses
- 4,000+ High-yield cases with fully scrollable DICOMs
- 500+ Expert case reviews
- Unlimited CME & CPD hours