Diagnosis Definition
- Vestibular schwannoma (VS), often referred to as “acoustic neuroma,” arises from the vestibulocochlear (8th cranial nerve) sheath; median age of presentation is 50 years
- VS is the most common extra-axial cerebellopontine angle (CPA) mass (70%–80%), followed by meningioma (10%–15%) and epidermoid cyst (5%)
- VSs may remain within the internal auditory canal (IAC) or extend into the CPA; those with both an IAC and CPA component are the most common
- Symptoms are related to compression of adjacent cranial nerves, brain stem, or posterior fossa structures; chronic asymmetric sensorineural hearing loss is more common than tinnitus or unsteadiness
- VS is unilateral in >90% of patients, with an equal incidence on the left and right
Imaging Findings
- Due to superior contrast resolution, MR imaging is the standard of care in evaluating VSs
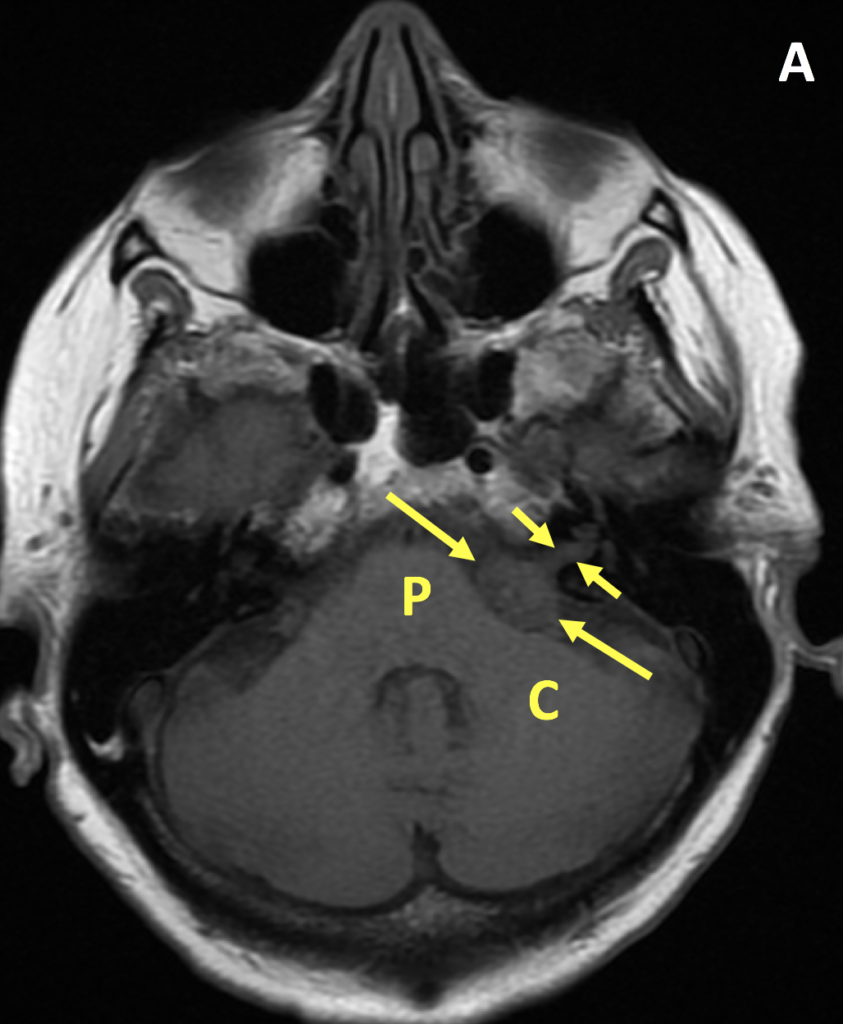
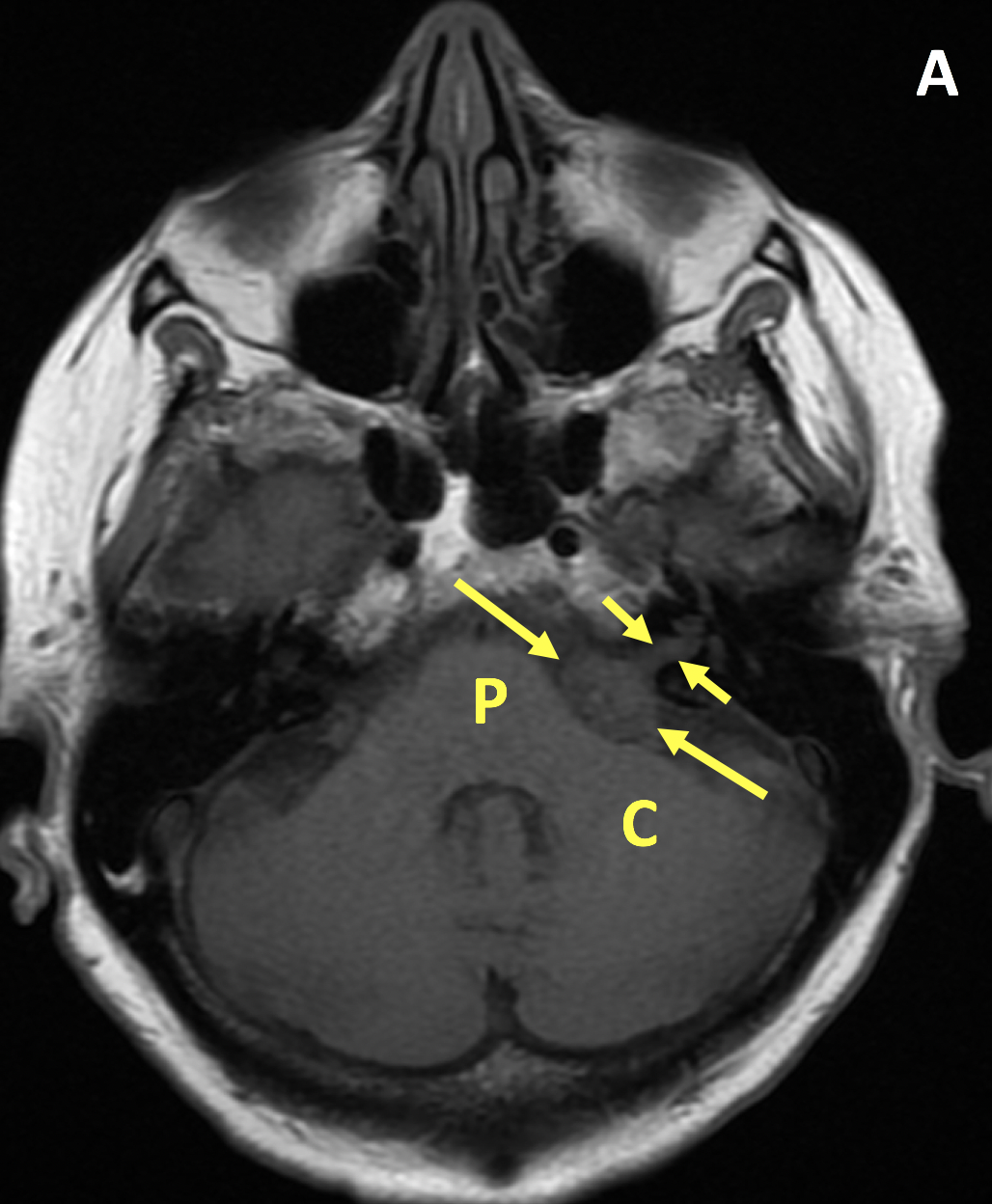
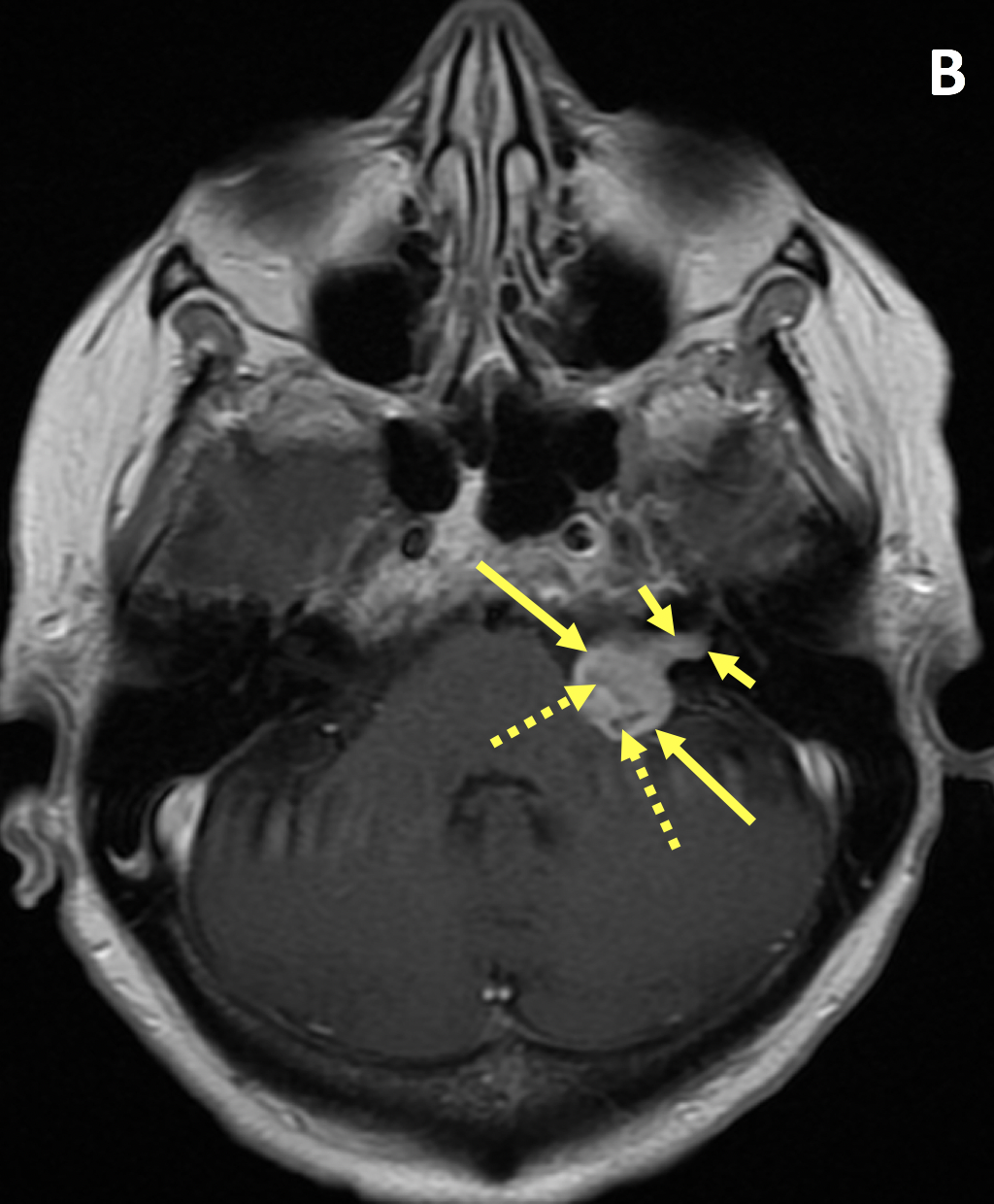
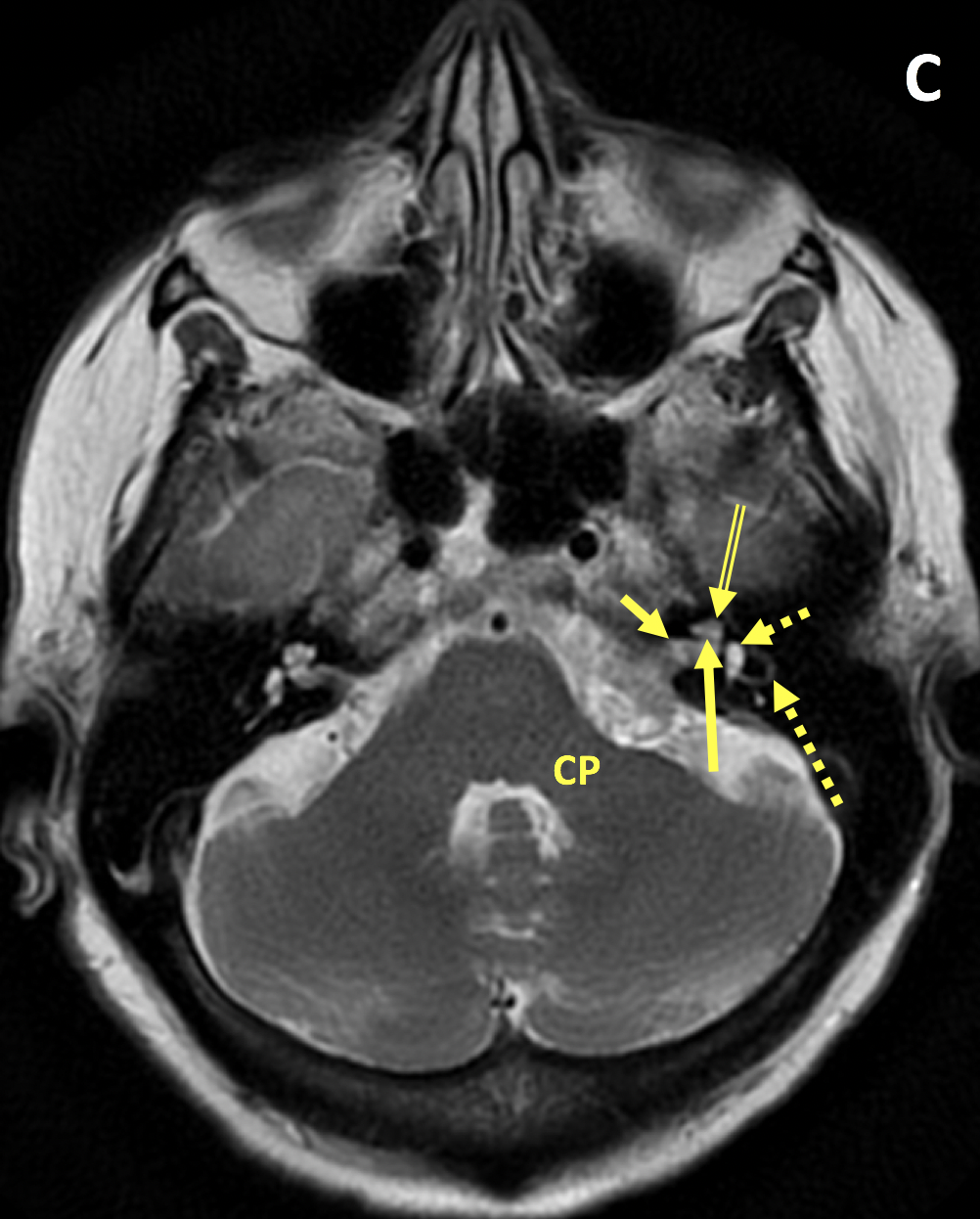
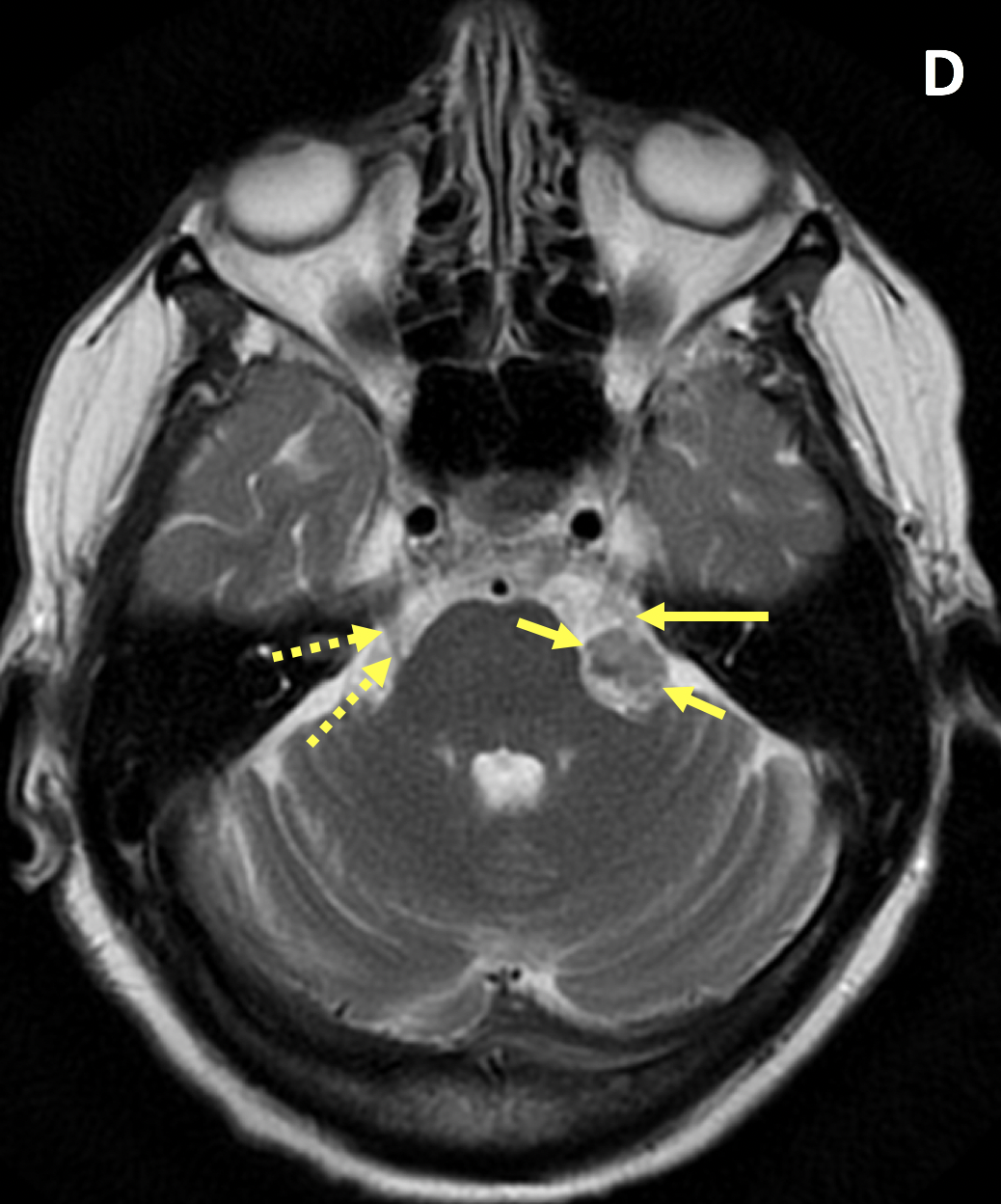
- VS is typically T1 isointense relative to the cerebellar parenchyma and demonstrates avid enhancement on postcontrast T1 images
- T1 hyperintense signal and susceptibility artifacts on T2* gradient-echo sequences may represent hemorrhage
- Larger VSs often demonstrate heterogeneous enhancement secondary to hemorrhage and cysts
- Important findings on MRI include mass effect on the middle cerebellar peduncle or extension to the cochlear aperture
Pearls
- CPA meningiomas are dural-based enhancing masses that grow along the petrous ridge and can extend into the IAC; they often have a characteristic dural tail and may be associated with bony changes
- Unlike a meningioma, a VS does not have calcifications
- Bilateral VSs are diagnostic of neurofibromatosis type 2
References
- Lin EP, Crane BT. The management and imaging of vestibular schwannomas. American Journal of Neuroradiology 2017; 38(11):2034-2043
- Gentry LR, Jocoby CG, Turski PA, et al. Cerebellopontine angle-petromastoid mass lesions: comparative study of diagnosis with MR imaging and CT. Radiology 1987;162:513–20
Case-based learning.
Perfected.
Learn from world renowned radiologists anytime, anywhere and practice on real, high-yield cases with Medality membership.
- 100+ Mastery Series video courses
- 4,000+ High-yield cases with fully scrollable DICOMs
- 500+ Expert case reviews
- Unlimited CME & CPD hours